This guidance was updated on 11 January 2021; click here to see the latest version
Wednesday 9 December 2020
COVID-19 vaccines
The UK was the first country to approve the use of a COVID-19 vaccine, which is being referred to as ‘The Pfizer vaccine,’ and vaccination with this started on the 8th December 2020. There is also another vaccine, known as ‘the AstraZeneca vaccine’ or ‘the Oxford vaccine,’ which has also been shown to be very effective at preventing COVID-19 and this is currently being assessed for approval. Other vaccines are in the pipeline.
Are these vaccines safe in people with HIV?
Some of the trials for the two most advanced vaccines have included a small number of people with HIV. There is no reason to think these vaccines will be less safe for people with HIV. Both include some of the genetic material from SARS-CoV-2 (the virus that causes COVID-19) but not the whole virus. This means they are not live vaccines and so are no less safe in people with damaged immune systems.
It is possible that people with HIV might not respond as well to the vaccine. This means that the vaccine might trigger a weaker response in people with HIV. We will monitor any new evidence as it is released and will update this advice if and when needed.
Who will get the vaccine?
People will receive the vaccine in strict order of priority based on their age, health, occupation, whether they live in a care or residential home and who they live with. Vaccines will be offered strictly based on these priorities. There is no way to jump the queue, and you will be contacted when your vaccine is due.
There are 9 priority groups: those in priority group 1 will get the vaccine first, followed by each in turn up until priority 9. After that the vaccine will be offered to everyone else (that is all the people not in priority groups 1-9).
Everyone with HIV is automatically in priority group 6 so you will get the vaccine earlier than many people. If your clinic thinks you are at higher risk you can be put into priority group 4, and get the vaccine sooner, but you will need to be added to a central NHS list to be put into priority group 4. We advise that the people at higher risk may include:
People with a CD4 count less than 50
People with a serious HIV-related illness (e.g. an opportunistic infection) in the last 6 months
People with a CD4 count between 50 and 200 with other issues that increase the risk of getting very sick, such as:
- Detectable viral load
- Low nadir CD4 (the lowest CD4 before starting HIV treatment)
- Other medical conditions associated with increased risk of severe COVID (such as asthma, COPD, diabetes, heart disease, kidney disease, liver disease, Parkinson’s disease, multiple sclerosis, motor neurone disease, conditions or drugs that suppress the immune system (e.g. steroid treatment), severe obesity.People with ‘multi-morbidity’ meaning that they have other health conditions that may increase the risk of getting very sick.
A full list of the different priority groups:
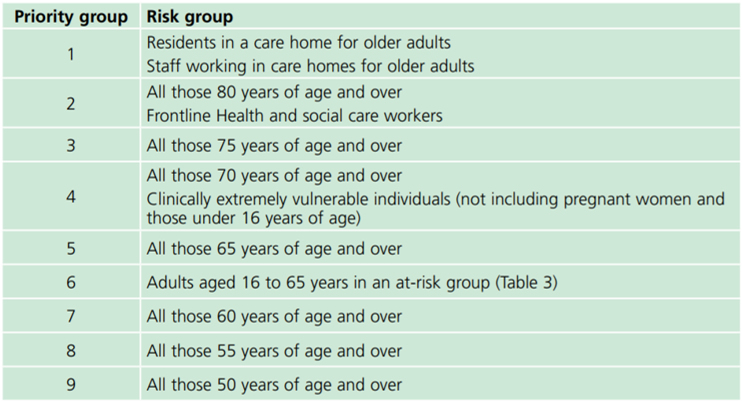
Will I have to have the vaccine?
No, nobody has to have the vaccine. However, we strongly recommend that everyone who is offered the vaccine accepts it. Although vaccine development has been very fast, it has been to the same high standards as any other vaccine trial and includes very careful monitoring of side effects. If anything changes we will update this guidance.
Does having the vaccine mean I don’t have to follow social distancing rules?
No. It will take many months to vaccinate everyone and it remains important to continue to wash your hands regularly, to wear a mask and to follow your local guidance about social distancing.
Notes: Safety data will be produced rapidly as the vaccine is rolled out. Please see MHRA website for the latest information.
For further information, please contact [email protected] or for media enquiries, please contact Jo Josh at [email protected] or +44 (0)7306 391875.



